Guest post by Stephanie Graves BSN, PHN, MA, Maternal and Child Health Coordinator for the Minneapolis Health Department
I ask you, is there cause for concern?
In January of 2020, the first reported case of the COVID-19 virus was announced in the United States in Washington state. Not even six weeks later, here in Minnesota, a COVID-19 case was confirmed. Although the person experiencing the illness began with symptoms in February, it took a few weeks to get lab results confirmed. From January until the official declaration of a public health emergency, many local health departments were gearing up for what was to occur, we just did not know how fast and devastating the COVID-19 pandemic would be on certain populations.
There was the usual, standing up an incident command center for public health emergencies and working with stakeholders, state and county government officials, first responders and health care providers. It was a good start in the early timeline of the COVID-19 pandemic, but then something was happening.
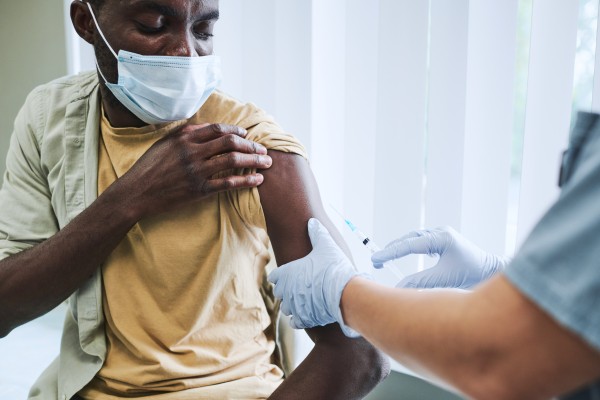
People from the BIPOC communities were dying at a much higher rate than that of the White population. What can we do, what should we do, who is responsible, are a few questions that public health professionals were asking leadership, stakeholders and ourselves. There were some good answers, but not anything we had not thought of previously. Later in the year, COVID-19 vaccine became available, however BIPOC community members continue dying at high rates.
A number of Minneapolis residents believe in vaccinations, however, there are a large number of BIPOC immigrant and refugee residents who are new to the Minneapolis area and have not connected to a medical home to date, nor felt it necessary to get immunized in general, especially not to prevent illness from a virus called COVID-19. Did this rise up as a cause for concern?
The answer of course was unequivocally, yes. Fortunately, we made a great decision (occasionally it happens), we got out of the way and went to community members. Through a NACCHO funded project, Equipping Local Health Departments to Address Vaccine Hesitancy, the Minneapolis Health Department received funding to conduct CDC’s Rapid Community Assessment. Through this process, our staff and trusted community messengers sat with community members and listened. Our department implemented listening sessions with elders, youth, and adults from BIPOC communities, including in the East African communities where vaccination rates are extremely low. Community members let us know their thoughts, feelings of distrust, fears, and beliefs around health, healthcare, and vaccinations. It is not the fault of particular communities for the vaccine rates being low, it is because of a multilayered system of inequities. Rather than community vaccine hesitancy, let’s see how we turn it around to focus on the true issue, racial and health inequities?
Equity lens
After a few of the community listening sessions, the conclusion to focus on the Somali community to provide accurate information and education on COVID-19 vaccinations was decided.
A major focus of our COVID-19 prevention work was to ensure communities struggling due to the inequities of the multiple bureaucratic health, economic, and social service systems were considered a priority, such as in the Somali community.
It is commonly recognized that COVID-19 disproportionately impacts and kills BIPOC, immigrant, incarcerated, and lower-income people at rates far higher than White, non-immigrant, and higher-income people. Furthermore, many of the strategies employed to reduce the health impacts of COVID-19 create unequal economic, cultural, and other impacts on these communities. The history of systemic racism at the systems and policy levels in employment, housing, health, and social services has perpetuated the inequitable exposures and outcomes that continue today.
Clearing the lens of equity
The work of providing COVID-19 and other accurate vaccination information continues into 2023 and beyond. Although the emergent time of the COVID-19 pandemic has passed, the work in BIPOC communities continues due to the low vaccination rates and continued health disparities. It will take time to clear the lens to have equity for all. As stated by a young Minneapolis resident, the Minneapolis Health Department is committed to ensuring we do nothing for the community without the involvement of the community. A number of our staff and leadership engage with stakeholders from health care, county and state public health, and social service systems to promote equity across disciplines and with policy makers.
The partnership we have with one of the Somali organizations has been instrumental. The partnership helps us keep abreast of what is needed to connect to families and which locations are best suited to provide immunization education and resource information. Our department continues to provide immunization education and outreach through communication outlets and direct staff contact, as well as community vaccination clinics.
Communication keys to success:
- Information is developed based on ongoing community input about questions and concerns.
- Quick responsiveness from SMEs, public information and outreach and trusted messengers to address community concerns.
- Clearly define information to be shared and ensure accuracy.
- Ensure in-language and in-culture approach when developing information.
- Plan ahead, by identifying timelines and resources needed (such translation/interpretation).
- Identify staff within public information and outreach who will become liaison and point of contact when working with SMEs and trusted community messengers.