Resilience Catalysts in Public Health
Resilience Catalysts in Public Health is a national collaborative and network of local health departments seeking to eliminate adversity, build resilience and foster equity through policy, practice, and program change. In collaboration with the Center for Community Resilience at the George Washington University (CCR) and the American Public Health Association (APHA), the Resilience Catalyst network utilizes the Community Resilience (CR) framework, developed at CCR by Dr. Wendy Ellis. The Community Resilience (CR) framework connects wellness to a local context focusing on place-based and systems-driven community and population health outcomes and is designed to be used by LHDs as a Public Health 3.0 strategy for the Chief Health Strategist
Public Health 3.0 in Action
Operating as Chief Health Strategists, local health departments are Resilience Catalysts, driving initiatives that foster integration of cross-sector and community services and community-wide prevention by leveraging a public health approach to prevent the Pair of ACEs, adverse childhood experiences and adverse community environments. Resilience Catalysts use the CR framework, with technical assistance provided by Center for Community Resilience at GWU and APHA, to conceptually connect place-based and systems-driven community context, population health outcomes, and policy following the Building Community Resilience process.
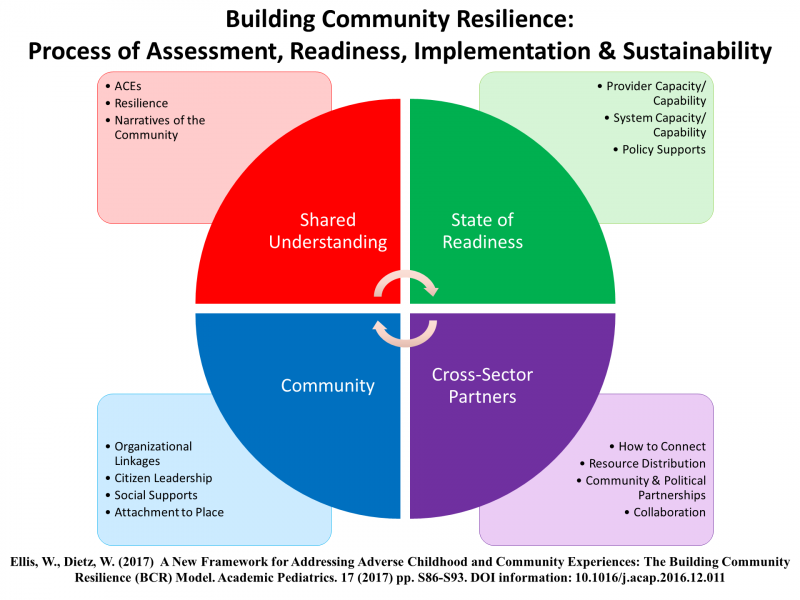
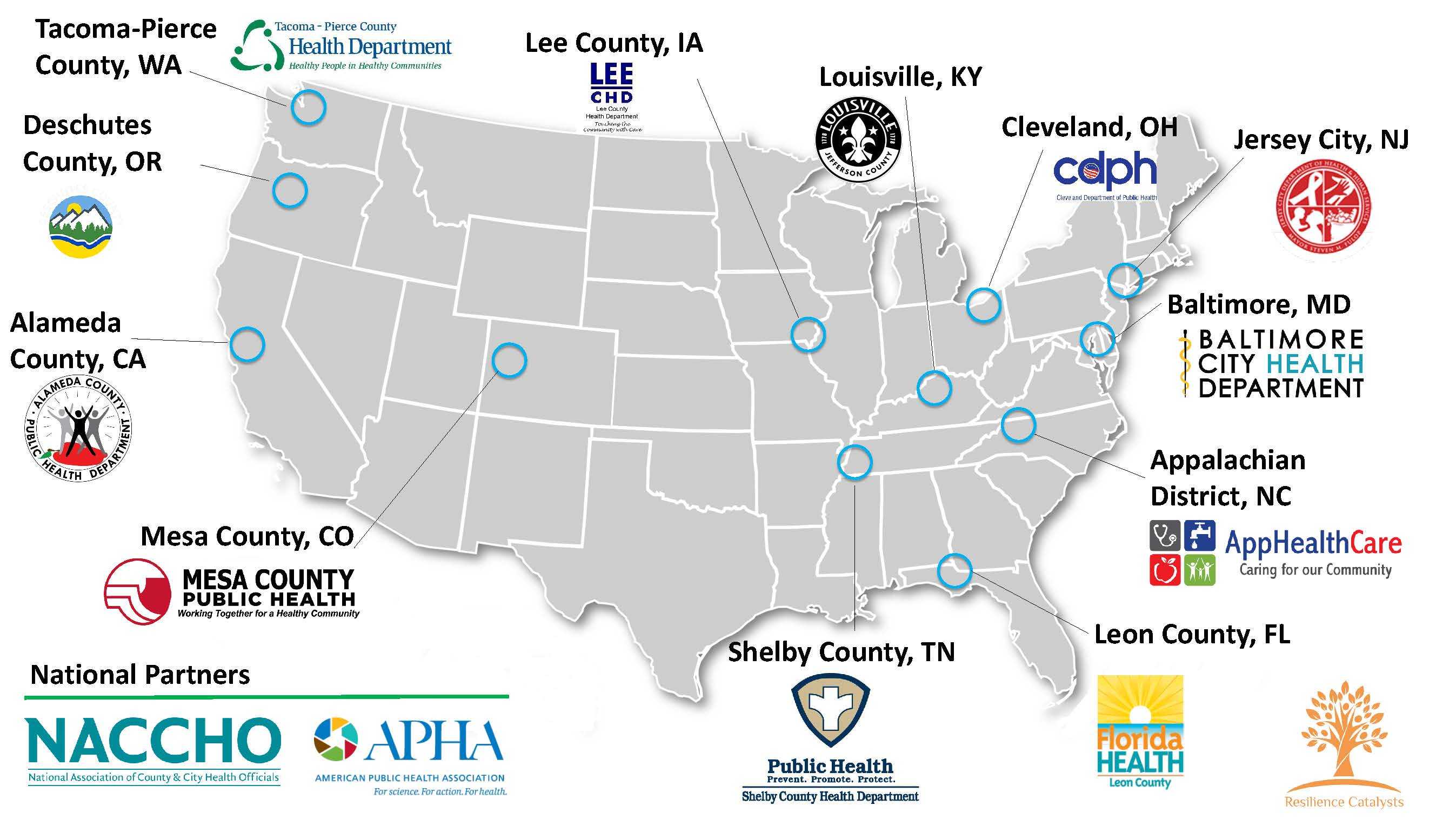
Resilience Catalysts in Public Health was launched in 2019 with four local health departments participating in our first cohort as network partners: AppHealthCare (NC), Cambridge Public Health Department (MA), Louisville Metro Public Health Department (KY), Mesa County Public Health (CO).
In fall 2020, we welcomed five local health departments to the Resilience Catalysts network: Alameda County Public Health Department (CA), Baltimore City Health Department (MD), Florida Department of Health- Leon County, Shelby County Health Department (TN), and Tacoma-Pierce County Health Department (WA).
We are pleased to announce of third cohort of local health departments to the Resilience Catalysts network: Cleveland Department of Public Health (OH), Deschutes County Health and Human Services (OR), Lee County Health Department (IA), and Jersey City Health and Human Services (NJ).
Acting as Chief Health Strategists, each local health department and their community partners have a theory of change and developed a systems dynamic model that maps relationships among multi-sector variables and identifies policy, practice change, and programming opportunities to address the Pair of ACEs, injury prevention, opioid misuse, suicide, and the impact of structural determinants on community characteristics, such as homelessness, juvenile incarceration rates, and educational attainment through a local lens.
Community Resilience: A Dynamic Model for Public Health 3.0: Read this new report in the January-February 2022 issue of the Journal of Public Health Management and Practice, which describes creating a model for Public Health 3.0 in order to define and measure community resilience as a method to measure equity, address structural racism, and improve population health.
Take a look at other NACCHO resources related to Public Health 3.0.
For more information about this program, please contact team members identified below.
There is also information and resources available from our partners at the Center for Community Resilience.
NACCHO Consulting
Tahlia Gousse
Consulting Specialist
JavaScript is required to reveal this message. / email hidden; JavaScript is required
Public Health Infrastructure and Systems
Alexandra Halprin
Program Analyst, Health Equity
JavaScript is required to reveal this message. / email hidden; JavaScript is required
Public Health Infrastructure and Systems
Brianna Aldridge
Program Analyst, Health Equity
JavaScript is required to reveal this message. / email hidden; JavaScript is required
