Healthcare-associated infections (HAIs) are a persistent and growing threat to the health of communities. To meet this threat head-on, more local health departments (LHDs) are building their capacity for HAI prevention and response. Enhancing LHD capacity can involve a wide variety of activities such as conducting exercises that test response plans, strengthening connections with healthcare partners to improve collaboration, and participating in formal training and professional development opportunities that build subject matter expertise. One such capacity building tool is the Certification Board of Infection Control and Epidemiology, Inc.’s (CBIC®) Certification in Infection Prevention and Control (CIC®) exam. According to CBIC, “The purpose of the certification process is to protect the public by providing standardized measurement of current basic knowledge needed for persons practicing infection control” and since eligibility requirements for the exam were updated in 2015, this has been increasingly available to LHD staff.
In the spring of 2016, NACCHO provided funding to 49 LHDs to purchase study materials and cover CIC® test costs for staff. These health departments received support for CIC® either through NACCHO’s CIC® scholarship program, HAI demonstration site project, or Lessons in INfection Control (LINC) Initiative. In late 2016 and early 2017, NACCHO distributed an assessment to the individuals at these health departments who took or planned to take the 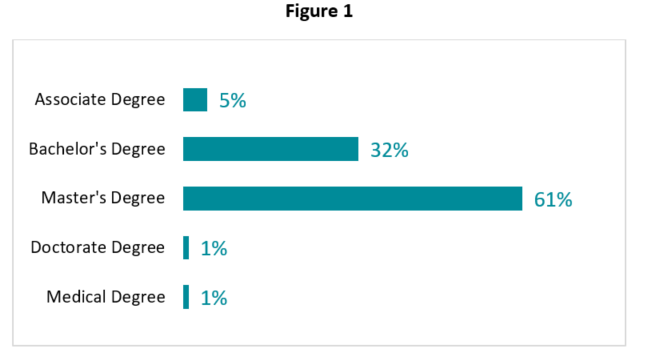 CIC® exam in order to understand the preparation process, participant lessons learned, and the impact of certification on the health department’s work. NACCHO utilized a mixed method survey disseminated via Qualtrics. 88 individuals completed the assessment for an 86% response rate. Of those who completed the assessment, the majority (61%) indicated that the highest level of school completed was a master’s degree (Figure 1) and the positions held by respondents included many roles related to infection prevention and control, including epidemiologists, public health nurses, communicable disease staff, and even included preparedness staff and leadership (commissioner).
CIC® exam in order to understand the preparation process, participant lessons learned, and the impact of certification on the health department’s work. NACCHO utilized a mixed method survey disseminated via Qualtrics. 88 individuals completed the assessment for an 86% response rate. Of those who completed the assessment, the majority (61%) indicated that the highest level of school completed was a master’s degree (Figure 1) and the positions held by respondents included many roles related to infection prevention and control, including epidemiologists, public health nurses, communicable disease staff, and even included preparedness staff and leadership (commissioner).
Assessment Results
NACCHO explored how LHD staff prepared for the exam in an effort to share lessons learned, strategies, and challenges with other LHDs. There are a variety of tools available and while many different resources were used to prepare for the exam, in-person courses and practice exams were identified as the most helpful (Figure 2).
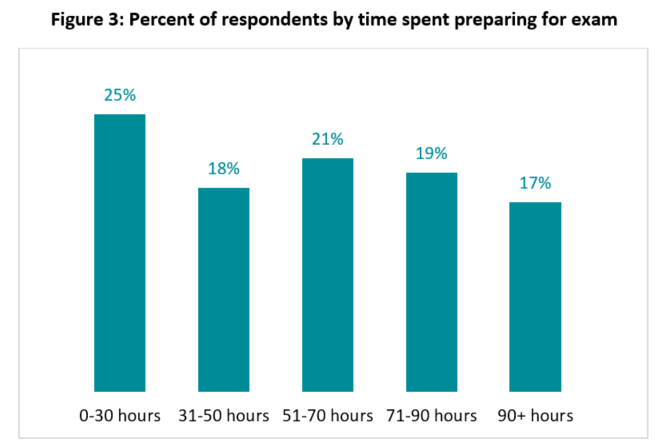
Although some people studied for 70 hours or more (Figure 3), more than half of those surveyed felt unprepared for the exam. Despite this, the majority (79%) of those who took the exam passed. Of those who passed, 59% studied for 50 or more hours. Of those who did not pass, one-third studied for 50+ hours. No one studied for more than 90 hours. Education level also correlated with who passed the exam (Figure 4).
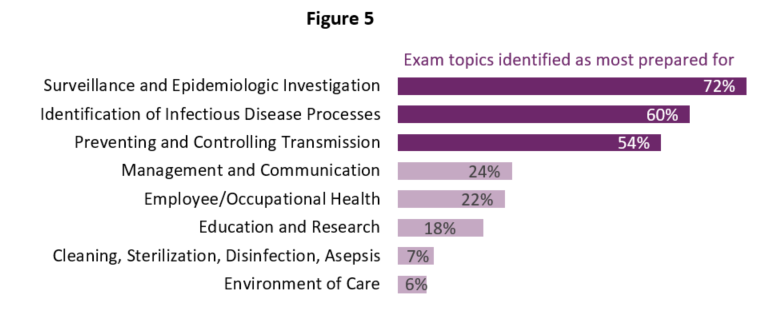
When asked what advice they would give to other LHD staff considering pursuing CIC®, survey respondents commented that while the exam must be taken within three months of registering, three months is not enough time to prepare and suggested starting preparation before registering to allow for at least six months to study for the exam. They noted the value of having support from your organization, leadership, and administration for both recognition of the effort and accomplishment, but also to possibly utilize work time for preparation. One other big theme among respondent recommendations was to identify the topics that are most challenging and focus time on those areas. Most participants found that the cleaning, sterilization, disinfection, asepsis, and environment of care sections were more challenging, as these topics tend to be much more clinical than LHD staff might see in their daily work (Figure 5).
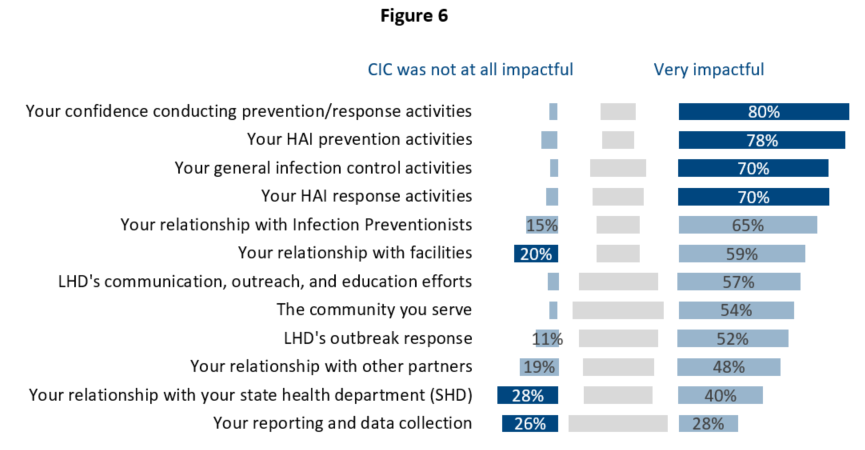
NACCHO has long had anecdotal evidence of the important role that CIC® can play as a tool for LHD capacity and used this survey to identify the areas where obtaining CIC® has impacted LHD HAI functions and activities. LHD staff who passed the exam were asked to reflect on what has changed since they obtained CIC® and they reported moderate to large impacts on a range of items. Most notably, participants indicated changes in staff confidence conducting HAI activities, relationships with infection preventionists, and a general impact on HAI prevention, infection control, and HAI response activities (Figure 6). An overwhelming 78% of respondents said CIC® was impactful overall.
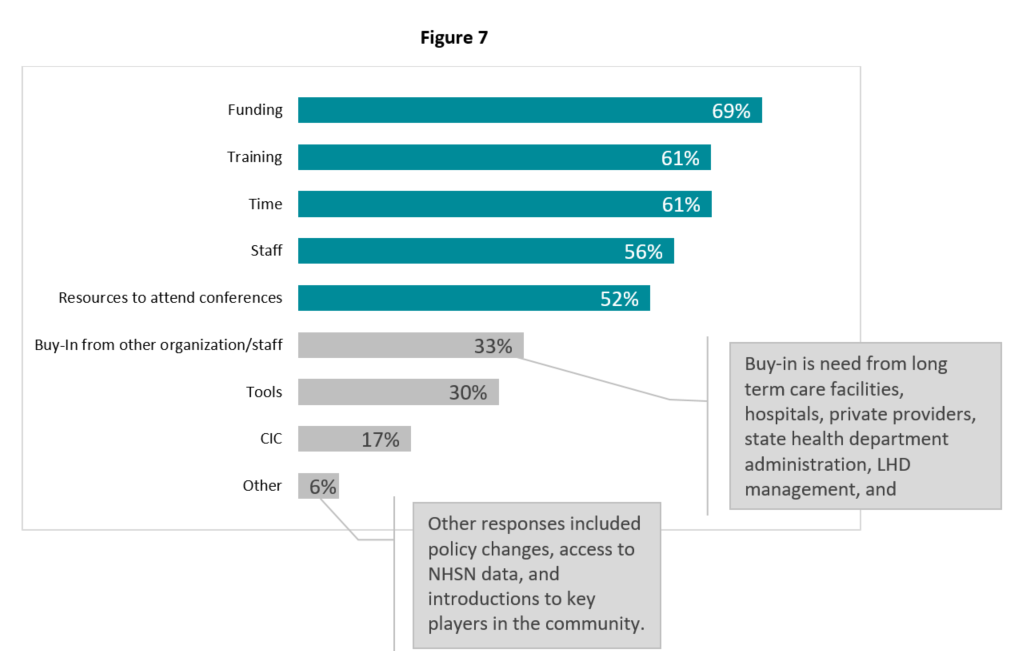
Staff who obtained CIC® stated that in addition to improving HAI investigation subject matter expertise, it had broader impacts on their work as well. It strengthened collaboration with partners and also served to indicate to partners that infection prevention is a priority for the health department. While CIC® has been a great resource for expanding LHD HAI capacity, staff who obtained certification also identified the need for improvements in technology, training, and communication with healthcare facilities to effectively address HAIs. When asked what LHDs and/or their staff need to become more involved in HAI infection prevention in the community, respondents indicated that funding, training, time, and staff are all priorities (Figure 7).
NACCHO asked what the Centers for Disease Control and Prevention, state health departments, and NACCHO could specifically do to support LHD HAI prevention efforts and the responses included:
- Bolster funding for LHDs, particularly for staffing;
- Support LHD capacity building and implementing training opportunities;
- Expand HAI reporting and increasing LHD access to data;
- Developand sharing guidelines, best practices, and tailored resources and promoting peer learning; and
- Increase communication and collaboration with LHDs.
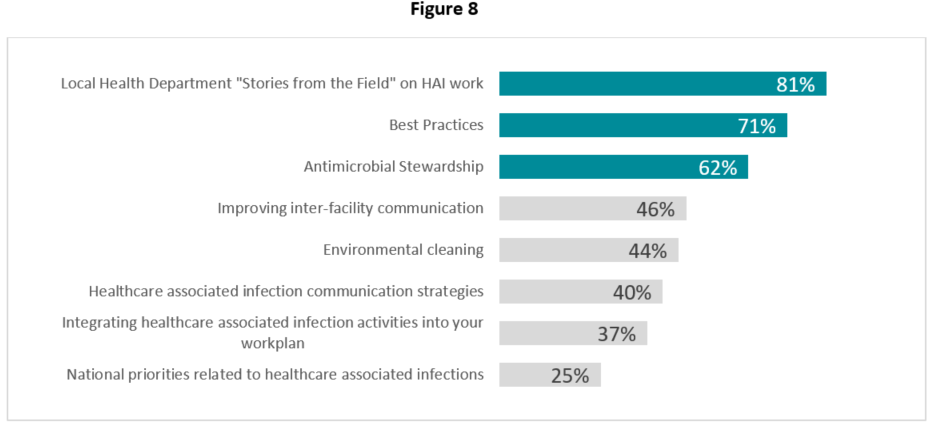
In addition, when asked what they would like to learn more about in relation to HAI prevention and response, experiences of other LHDs, best practices, and antimicrobial stewardship were the most commonly identified themes (Figure 8).
This assessment reaffirmed for NACCHO that CIC® is a valuable tool for LHD HAI prevention and response and that continuing to advocate for CIC® for LHDs – in terms of access, training, and funding – should be a priority. It also reinforced that CIC® is just one tool in the toolbox of effective HAI public health response and that ongoing efforts to support LHD capacity are needed. Local health departments can play a vital and diverse role in HAI prevention and response by identifying and investigating HAIs and providing recommendations for control measures. They can also play a critical role as conveners, connecting and coordinating with healthcare facilities that may share patients; collaborating with infection preventionists; and supporting surveillance and outbreak response activities. Building local capacity makes prevention and response more effective, strengthens initiatives to combat HAIs at the state and federal level, and creates opportunities for improved health outcomes across entire communities.