COVID-19 has had a profound impact on our society beyond the physical toll on those infected with the virus. It has also caused restriction of resources for non-COVID conditions, economic upheaval, and interrupted care on chronic conditions. One of the most significant impacts, however, has been the toll that COVID-19 has taken on mental health and substance use disorder (SUD). According to an MMWR issued in August 2020, almost 41% of respondents reported a mental health condition such as anxiety or depression, 30% reported symptoms of trauma- and stressor-related disorder, and 26% reported starting or increasing substance use to cope with stress related to COVID-19. In April of 2020, a federal emergency hotline for people in emotional distress registered a more than 1,000 percent increase in calls, compared with April 2019 and suicidal ideation has increased as well, particularly among young adults.
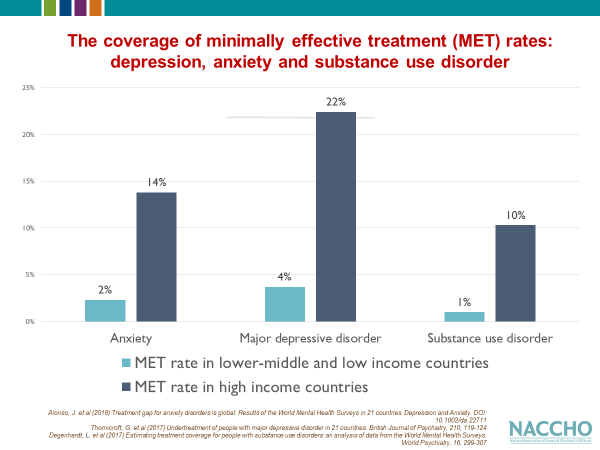
This increase in mental trauma, depression, anxiety, and substance use is straining a chronically underfunded and under-resourced mental healthcare system. According to the World Health Organization (WHO), even before the pandemic in high-income counties, coverage for minimally effective treatment for anxiety, major depression disorder, and SUD is at 14%, 22%, and 10% respectively. The pandemic has resulted in a widening care gap for mental health and SUD services, where the supply of specialists available cannot meet the demand of those who need their services. According to an interview with Ken Duckworth, Chief Medical Officer of the National Alliance on Mental Illness with the New York Times, “It takes eight months to explode demand, but several years to make a social worker.”
However, relying on the supply of social workers and other specialists is not the only solution to this growing challenge. There are opportunities for non-specialists to provide mental health and SUD care for people to help close the care gap that currently exists.
Utilizing non-specialists to provide basic mental health care has been a common practice for low- and middle-income countries and research has shown it can be an effective strategy. A systematic review of 29 studies completed by the WHO, showed that mental health training for generalized health workers is a cost effective and well-accepted way to improve clinical practice and better mental health patient outcomes. According to a policy brief by the Public Health Foundation of India, focusing on non-specialists for mental health care can improve anxiety and depression and they recommended expanding their cadre of frontline non-specialist health workers for identification and treatment of depression at the national level. The WHO has a robust mental health department that provides guides, manuals, and toolkits to address the mental health needs of people living in low-, middle-, and high-income countries around the world, focusing specifically on providing non-specialist options for care.
Given the current gap in mental healthcare that exists in the United States, due in large part to the expansion of demand due to COVID-19, NACCHO sees this global approach of focusing on non-specialists as an opportunity to address this challenge at the local health department (LHD) level. NACCHO’s new Global Health team works to increase the bidirectional sharing of global health approaches and provide opportunities for U.S. LHDs to adopt and adapt solutions from around the globe to address challenging health issues that they are experiencing in their own communities. NACCHO’s new Global team is working with Dr. Shekhar Saxena, Professor of the Practice of Global Mental Health at Harvard University and former Director of the Department of Mental Health and Substance Abuse at the WHO to introduce selected LHDs to the mental health resources made available by the WHO, and support them in developing an implementation and sustainability plan to address the unique needs of their own communities
This pilot program will allow NACCHO to understand how to better adopt and adapt global resources to address local public health needs. As we continue to grapple with the direct and indirect effects of the COVID-19 pandemic, global health can offer strategies and opportunities that LHDs can use to address and improve the health of their communities.



